Blog
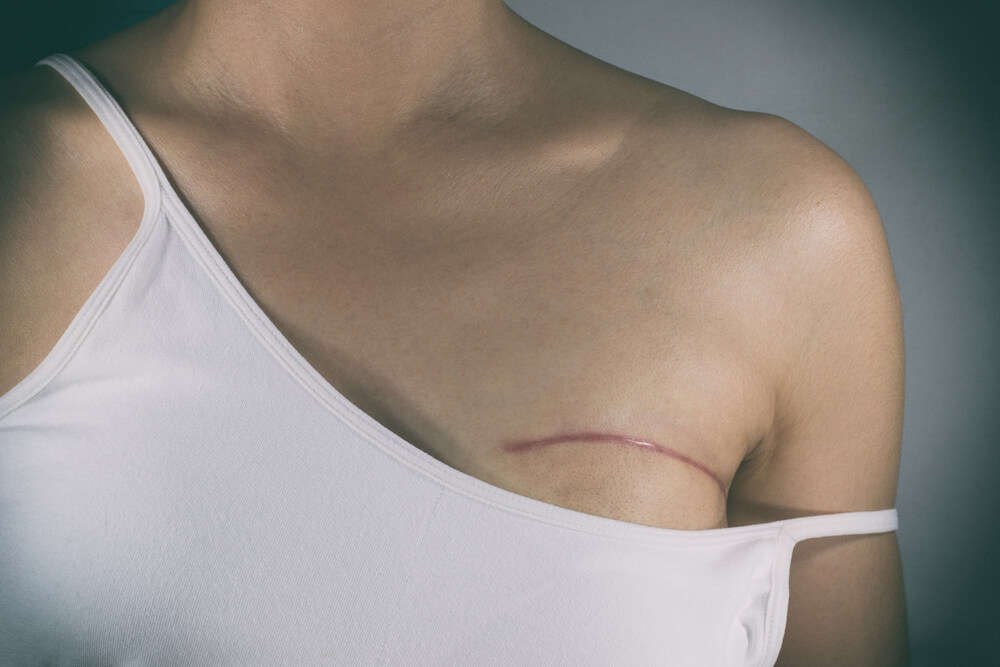
Understanding and Managing Lymphedema After Breast Surgery
The journey through breast cancer entails many changes, some of which transcend beyond the disease. A potential outcome of breast
Nutrition and Its Impact on Breast Health
What you choose stands at the intersection of overall health and breast health. An optimal diet is the frontline defense,
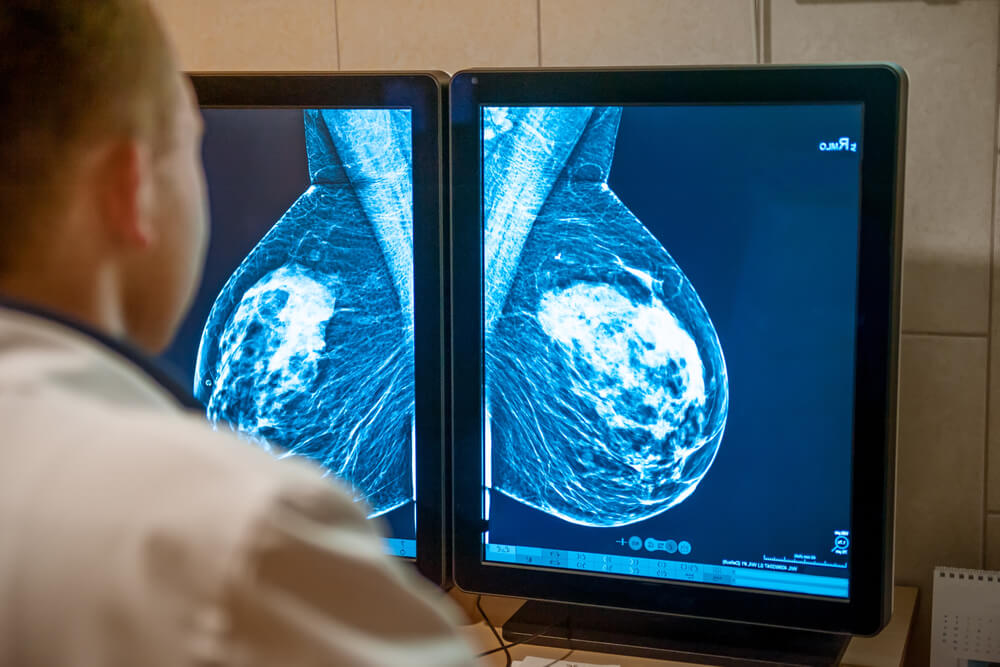
What is a Breast MRI
A Breast MRI, short for Magnetic Resonance Imaging, is an advanced medical imaging technique used primarily to detect breast cancer,
The Most Common Causes of Reduced Breast Milk Supply
When a woman gives birth, her body naturally begins the process of lactation, producing nourishing breast milk for her newborn.
What is Mammary Duct Ectasia?
Mammary duct ectasia, often referred to simply as duct ectasia, is a frequently misunderstood and usually overlooked condition that primarily
How Do Breasts Change During Menopause and How to Mitigate It
As women journey through the natural life transition of menopause, they often encounter a myriad of changes, both physical and
What Is Breast Implant Illness
Welcome to our Breast Care Center Miami, where your well-being is our top priority. In recent years, there has been
Everything You Should Know About Modified Radical Mastectomy (MRM)
A Modified Radical Mastectomy (MRM) is a procedure that plays a vital role in the comprehensive management of breast cancer.
Common Breast Problems Related to Breastfeeding
Breastfeeding is a beautiful and natural aspect of motherhood, fostering a unique bond between a mother and her child. However,
Patient Feedback
Rafaela H.
Great surgeon, very caring and compassionate.
Selena P.
I just met him today and he was amazing! Highly recommend him! Good vibes
Bob D.
Simply the best!